The primary survey is the initial assessment and management of a trauma patient.
Use a systematic approach based on <C> ABCDE(11, 12) to assess and treat an acutely injured patient. The goal is to manage any life-threatening conditions and identify any emergent concerns, especially in a spinal trauma patient who may present with other multisystem injuries.
All patients with a mechanism of injury likely to have induced SCI must have an appropriately fitted and sized collar placed and inline immobilisation implemented.
Regular assessment is crucial in SCI trauma patients as developing cord oedema may cause significant changes in neurological function.
- Catastrophic haemorrhage
- Airway with in-line spinal immobilisation
- Breathing
- Circulation
- Disability (neurological)
- Exposure and environment
Catastrophic Haemorrhage
Assess for catastrophic haemorrhage
- Identify any large volume external blood loss.
- Provide immediate management as required, consider; direct pressure, haemostatic dressings and tourniquets.

Airway with cervical spine protection
Early and safe airway management in the SCI patient can make a crucial impact to long-term patient outcomes and functional deficits.
Assess for airway stability
Attempt to elicit a response from the patient.
Look for signs of airway obstruction (use of accessory muscles, paradoxical chest movements, see-saw respirations).
Assess for displaced dentures, especially in the older persons cohort.
Listen for any upper-airway noises, breath sounds. Are they absent, diminished, or noisy?
Spinal patients are at particular risk of passive regurgitation and subsequent aspiration. High cervical injuries potentiate loss or compromise of both gag and cough responses. (Nasogastric tube insertion is highly recommended although consideration of intubation and inherent airway protection should be considered prior to insertion.)
Attempt simple airway manoeuvres if required
Open the airway using a chin lift and jaw thrust whilst avoiding neck extension to protect the C-spine.
Suction the airway if excessive secretions are noted or if the patient is unable to clear their airway independently.
Insert an oropharyngeal airway (OPA) if required.
Caution: Nasopharyngeal airways (NPA) should not routinely be inserted in patients with a head injury in whom a base of skull fracture has not been excluded.(13) In the setting of airway obstruction, or failure to oxygenate, then an NPA can be inserted if delay to definitive airway management.
Caution: Bradycardia or cardiac arrest as a response to tracheal suction, endotracheal intubation, laryngoscopy or other tracheal stimuli are found mainly during the acute phase, in patients with high complete cervical SCI, and this problem usually resolves within the first 2-6 weeks after SCI.(14)
Maintain full spinal precautions if indicated
Suspect spinal injuries in all polytrauma patients. Ensure cervical collar, head blocks and in-line immobilisation is maintained throughout patient care.
Secure the airway if necessary (treat airway obstruction as a medical emergency)
Consider early intubation if there are any signs of:
- Decreased level of consciousness, unprotected airway, an uncooperative/combative patient leading to distress and further risk of injury.
- Apnoea or respiratory failure due to paralysis.
Intubation of the patient while maintaining full spinal precautions requires skill and a high level of teamwork.
Manoeuvres to open the airway that mobilise the cervical spine, such as a neck tilt, are contraindicated. Only jaw thrust and chin lift should be utilised.
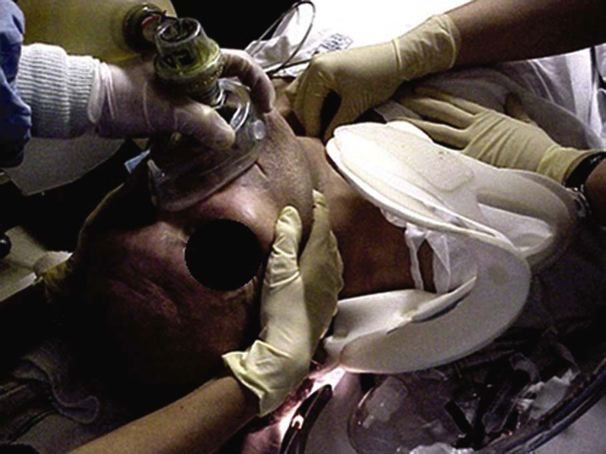
Image used with permission from Jeffery Rosenfeld, Practical management of head and neck injury, 2012, Sydney, Elsevier Australia
Manual in-line cervical stabilisation must be maintained while the cervical collar is removed to facilitate intubation. A second assistant may apply cricoid pressure over the cricoid cartilage ring while intubation is performed. The use of external laryngeal manipulation may be an effective procedure to mobilise the airway and to facilitate vocal cord identification. Prophylactic, pre-treatment of quadriplegic and high-paraplegic patients with atropine is indicated prior to airway management due to unopposed vagal tone and the risk of bradycardia during pharyngeal stimulation.
Breathing and ventilation
Assessing for adequate ventilatory effort is essential.
Administer high flow oxygen and record the oxygen saturation (SpO2).
Patients with a spinal injury may have respiratory compromise relative to the level of injury and spinal cord compromise, remembering that the diaphragm is innervated by cervical nerves 3, 4, and 5. Breathing and ventilation may be compromised by direct pulmonary injury or aspiration. They may present with an inadequate cough reflex, hypoventilation, and apnoea. Rising spinal cord oedema may result in progressive loss of diaphragmatic function.
Assess the chest
Be mindful that thoracic injuries may have also occurred.
Count the patient’s respiration rate and note the depth and adequacy of their breathing.
Auscultate the chest for breath sounds and assess for any wheeze, stridor, or decreased air entry.
Paradoxical breathing, a sign of high spinal injury, results from activation of the diaphragm while thoracic muscles remain paralysed, causing the thorax to cave in (respiratory movements in which the chest wall moves in on inspiration and out on expiration, in reverse of the normal movements).

Circulation with haemorrhage control
Assess circulation and perfusion
- Check the heart rate and blood pressure.
- Inspect for any signs of external haemorrhage and apply direct pressure to any wounds.
- Insert two large-bore peripheral intravenous (IV) cannulas. If access is difficult, consider central or intraosseous insertion if the equipment/skills are available.
Management of volume resuscitation is important in spinal patients and hypotension should be avoided; a general guide is to maintain a systolic blood pressure of above 90 mmHg and targeting a MAP of 85-90mmHg.(15, 16) It is important not to assume that hypotension in a patient with SCI is solely as a result of their cord injury without excluding other causes such as haemorrhage.
Expect hypotension and bradycardia associated with spinal shock in those with lesions at or above T6 neurological level of injury.
Additionally, neurogenic shock may cause a bradycardia, contributing to hypotension, and may require treatment with medication.
A heart rate less than 45 bpm and blood pressure under 90 mmHg require treatment in consultation with ARV and the receiving unit.
Consider the need for FAST (Focused Assessment with Sonography in Trauma) if available and if staff are trained in its use. FAST is used primarily to detect pericardial and intraperitoneal blood, and it is more accurate than any physical examination finding for detecting an intra-abdominal injury.
If the patient is haemodynamically stable and there are no signs of significant internal bleeding, then FAST may be delayed until the secondary survey.
Disability: neurological status
Assess level of consciousness
Complete an AVPU assessment (Alert, responds to Voice, responds to Pain, Unresponsive). A more detailed neurological assessment using the GCS will be performed in the secondary survey.
Until ruled out by appropriately qualified clinical personnel (and where necessary with supportive radiological examination), major trauma patients should be considered at risk of spinal injury.
Identifying a cervical spinal injury in primary assessment is important. Priapism, diaphragmatic breathing, and loss of anal tone are key signs of high spinal cord compromise.
Combative patients should not be physically restrained due to the increase in leverage and potential for further injury. Sedation, intubation, and ventilation may be indicated to manage severe agitation.
Check pupillary response.
Test blood sugar levels
Ensure that any alterations in level of consciousness are not related to a metabolic cause.
Exposure/environmental control
Remove the patient’s clothing and any jewellery in order to be able to fully assess all areas of the body.
An SCI patient can become hypothermic due to the loss of autonomic regulation, so it is important to monitor their temperature and keep them in a warm environment.
